Understanding Duodenal Atresia
What is duodenal atresia?
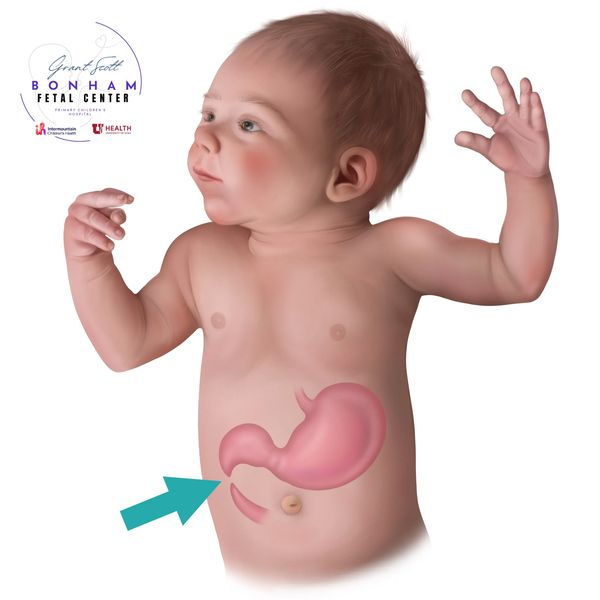
Duodenal atresia, sometimes referred to as congenital duodenal obstruction, is a condition in which the duodenum, or the first part of the small intestine just beyond the stomach, is blocked or does not form properly. Because of this blockage, food and stomach contents cannot pass into the rest of the intestines.
- It occurs in approximately 1 in 5,000–10,000 live births and develops early in pregnancy
- It is commonly associated with Down syndrome or Trisomy 21, seen in about 25–35% of cases
- Other congenital anomalies, especially cardiac defects may also be present
(Pic: child with duodenal atresia)

Fetal Center: the first step in care
Multidisciplinary Evaluation: meet with MFM specialist, pediatric surgeon, neonatologist, and other experts who will care for your baby
Comprehensive Imaging: detailed ultrasounds and other tests when indicated to assess your baby's condition and help plan treatment
Coordinated Delivery Planning: our team works to ensure your baby receives immediate specialized care at birth
How is duodenal atresia prenatally evaluated?
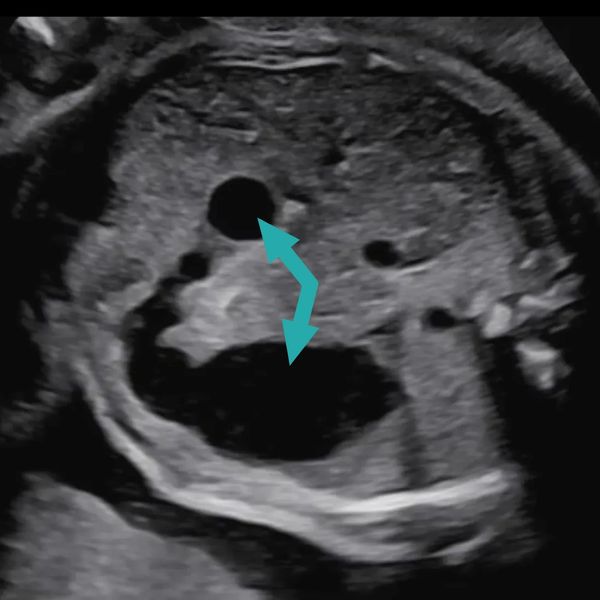
Duodenal atresia is often detected before birth on routine prenatal ultrasound, with the following findings:
- “Double bubble” sign (fluid-filled stomach and duodenum)
- Polyhydramnios (excess amniotic fluid), because the baby cannot swallow and absorb fluid normally
When suspected prenatally, additional evaluation may include:
- Detailed anatomic ultrasound to look for other anomalies
- Fetal echocardiogram to assess the heart for a congenital heart defect which occurs in about 30%
- Genetic counseling and testing (if desired)
(Pic: ultrasound of a fetus with duodenal atresia, with the arrows showing the "double bubble" sign)

Neonatal Intensive Care
Babies with known duodenal atresia should be delivered at our center where a neonatal intensive care unit (NICU) is available that specializes in the care of these infants and where a pediatric surgeon can immediately evaluate your child. The neonatologist is a specially trained pediatrician that will manage your baby’s medications, feeding, and daily needs while in the NICU.
Once the child is born, a neonatologist will evaluate the baby and make sure the heart and lungs are working appropriately. A tube placed through the mouth (oral gastric or OG) into the stomach to suck out air and fluid to prevent your baby from choking contents into the lungs.
Your baby will receive fluids and antibiotics through a special IV called a PICC line, typically placed in one of the limbs. Because the child will not be initially allowed to eat, they will also receive nutrition through the PICC line called TPN, or total parenteral nutrition. TPN contains protein, fat, sugar, vitamins, and minerals and will meet all your baby’s nutritional needs
Feedings usually begin 5 - 7 days after surgical repair, typically at a low level, gradually increasing to goal.
A child with a duodenal atresia is typically in the hospital for 4 - 6 weeks, although this may be longer if an associated heart defect or genetic disorder is also present
What is the treatment for duodenal atresia?
The definitive treatment for duodenal atresia is surgical repair.
The most common operation is a duodenoduodenostomy, in which the surgeon connects the two healthy ends of the duodenum to bypass the blockage.
- Typically performed within the first few days of life
- May be done via open or minimally invasive (laparoscopic) techniques, depending on the situation and surgeon expertise
(Pic: surgical team performing surgery)
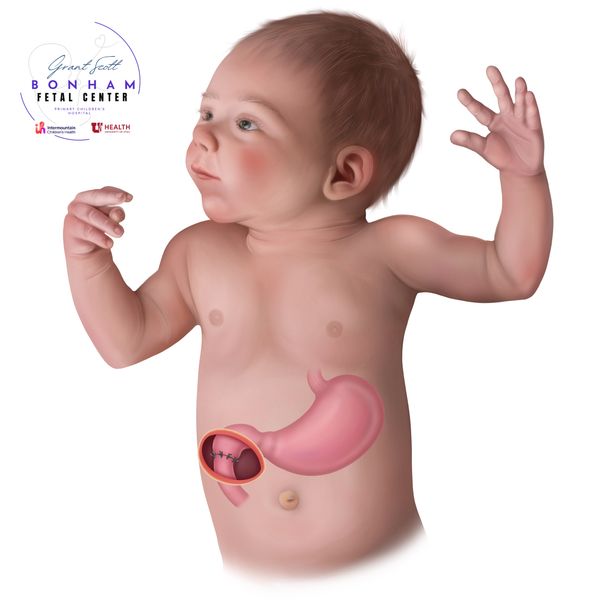
Open duodenal atresia repair
The open surgical repair of duodenal atresia is typically performed through an incision in the right upper abdomen. Here, the surgeon connects both ends of the duodenum so the stomach and empty appropriately. In about 15% of case, malrotation of the intestines is also found. If so, the surgeon will also perform a Ladd's procedure, where the intestines are put into a place that won't result in twisting or volvulus in the future. This doesn't significantly add to the overall time or complexity of the procedure.
(Pic: child undergoing open repair of duodenal atresia)
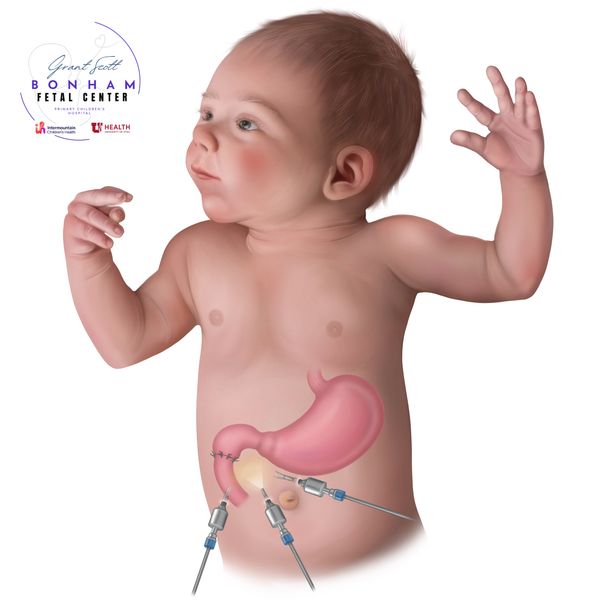
Laparoscopic duodenal atresia repair
In some cases, a less invasive approach can be taken and the repair can be performed laparoscopically, or through 3 small incisions. Here, the surgeon uses a camera and thin instruments to put the two ends of the duodenum together.
Recovery is usually dependent on how quick the stomach recovers as well as any other anomalies, such as congenital heart disease, the child might have.
(Pic: child undergoing laparoscopic repair of duodenal atresia)

Outcomes and Long-term outlook
The prognosis for isolated duodenal atresia (without major associated conditions) is excellent, with survival rates greater than 95%.
In general, long-term outcomes are very good and most children are able to:
- Feed normally
- Grow and develop appropriately
- Do not require long-term dietary restrictions
Outcomes depend more on associated conditions (such as a heart disease or genetic disorder) than on the intestinal repair itself
Our Partners




Copyright © 2025 Grant Scott Bonham Fetal Center - All Rights Reserved.
Phone: (801) 662-6474
Fax: (801) 442-0570
info@grantscottbonhamfetalcenter.org